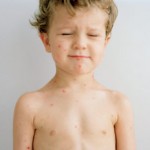
 Last Thursday (when I actually started this post!) I was getting my 3-and-a-half year old daughter dressed for school when I noticed a spot– no, make that four spots– on her stomach. My first thought was, “Oh no, chickenpox!” She’d had the vaccine, but according to studies less than 5% of kids get “breakthrough infections” which are mild and usually result in only a few days of a low-grade fever and a few spots.Turns out she was one of those…
Last Thursday (when I actually started this post!) I was getting my 3-and-a-half year old daughter dressed for school when I noticed a spot– no, make that four spots– on her stomach. My first thought was, “Oh no, chickenpox!” She’d had the vaccine, but according to studies less than 5% of kids get “breakthrough infections” which are mild and usually result in only a few days of a low-grade fever and a few spots.Turns out she was one of those…
To find out whether what she had was actually chickenpox (or just some random virus… or crazy bug-bite attack??) I (naturally) turned to Dr. Sears, whom I consult on all medical and child-raising topics. (I do have a great family doctor, but this is so much more convenient!)
Dr. Sears advises that for straightforward cases of chickenpox, you don’t really need to see or even call the doctor. Basically you just need to wait it out and treat the symptoms (itching, fever) rather than treat the chicken pox itself (it’s a virus, you can’t do much about it.)
Here’s some important info from the good doctor:
The key to diagnosing chickenpox. Watch the progression of spots from bumps to blisters to crusts, and to have a mix of all three types during the illness. Very important note – it is nearly impossible to diagnose chickenpox on day 1, and still difficult to know for certain on day 2. Therefore, do not bring your child into the doctor on day 1 or 2 and expect a definite diagnosis. If you think its chickenpox, then quarantine your child until day 3. If the spots have progressed as described above, then you probably don’t even need a doctor to confirm it.
Dr. Sears suggests: If you suspect your child may have chickenpox draw a circle around a few of your favorite spots. If they all become blisters within a day, they are probably chickenpox. If they don’t change dramatically then chickenpox is unlikely.
Well, it’s now four days later and it really was a mild case, thank God! Although she was itchy (and refused to allow me near her with calamine lotion!) she didn’t have a fever at all, and has only around 20 spots (mostly on her stomach, back, and head). There have been no new spots since Friday and I think it’s pretty much done. I don’t even think she’s contagious anymore, so back to school tomorrow… phew!
Here is some more chickenpox advice from Dr. Sears:
You should see your doctor if:
- You are not sure about the diagnosis after two or three days have passed.
- An infant 2 months or younger catches chickenpox.
- Your child has a weakened immune system such as from an immune disorder or from taking steroid medication.
- The mother of a newborn baby breaks out in chickenpox less than 3 days after the birth.
- Your child has fever more than five days.
- Your child develops a moderate to severe cough.
- Severe headaches develop even when fever is controlled (high fever can cause headaches, which is not worrisome).
- Significant dizziness (spinning feeling) occurs.
- Severe headaches with vomiting and stiff, painful back of the neck or spine.
- Any spots become infected with redness spreading outward from the spot with puss draining out.
- Your child has spots on the upper or lower eyelids, or has red, painful eyes.
- You are pregnant, are exposed to chickenpox, and have never had the illness or the vaccine.
You should page your doctor after hours if:
- Your child has severe headaches with vomiting and stiff, painful back of the neck or spine.
- If your child seems seriously and unusually ill.Otherwise, chickenpox is not a serious illness and rarely warrants paging the doctor after hours.
HOW LONG IS MY CHILD CONTAGIOUS?
Your child is contagious starting the day before fever or spots appear, until 24 hours after all the blisters have crusted over. This usually takes about 7 days from beginning to end.
HOW DID MY CHILD CATCH CHICKENPOX?
It is passed through the saliva, coughing secretions, and direct touch. In general, you must either be living in the same house, or play indoors in close face-to-face contact for more than 5 minutes, or have close face-to-face or physical contact outdoors in order to catch the illness.
MY CHILD WAS EXPOSED TO CHICKENPOX. HOW LONG UNTIL HE MAY BECOME SICK?
The incubation period (the time from when your child is exposed to the time he will break out in spots) is generally 14 days. It can be as early as 7 days and as long as 21 days. If three weeks pass from your child’s exposure, than he is in the clear.
I AM PREGNANT AND WAS EXPOSED. CAN THIS HARM THE BABY?
If you had chickenpox previously, or have had the vaccine, then you should be immune and there is virtually no risk to the baby. If you never had chickenpox or the vaccine, then you should contact your obstetrician right away to discuss possible options for preventing the illness.
I HAVE A NEWBORN AND MY OLDER CHILD WAS JUST EXPOSED TO CHICKENPOX, OR JUST BROKE OUT WITH CHICKENPOX. WHAT SHOULD I DO?
If your older child was exposed, then try and keep the baby away from him during the 7 to 21 day period after exposure. This may be tough, but it’s important. Breastfeeding will help provide your baby with some immunity. If your older one breaks out in chickenpox, then just quarantine him until no longer contagious as above. If your newborn infant was exposed before you knew the situation, there is really no way to prevent the illness, yet most likely your newborn carries your immunity to chickenpox.
TREATING CHICKENPOX
Treat the itching:
- Cut the fingernails
- Benadryl (an over-the-counter antihistamine) is very effective in decreasing the itching. Use it as needed. Click on benadryl for dosing.
- Oatmeal baths: Aveeno or other brands can be purchased at the store. This can soothe the itching.
- Cool washcloths may help.
Treat the fever:
- DO NOT USE ASPIRIN DURING A CHICKENPOX INFECTION. This can cause a serious reaction.
- Acetaminophen (Tylenol) and ibuprofen (Motrin or Advil) can be used to treat the fever.
- ONE IMPORTANT NOTE: Do not treat the fever if it is below 101 and your child is feeling relatively okay. Studies have shown that children do better overall when some fever is allowed to continue during this illness. Therefore, only treat the fever if it is high, or you child is bothered by the fever.
Medications to help decrease or shorten the illness:
Acyclovir is an antiviral medication that has some effect against chickenpox. If started within 24 hours from the onset of rash, it can shorten and lessen the illness. It is not, however, recommended for routine use in normal, healthy children because its benefit is often not very significant.
Acyclovir is recommended to be used for people who are at higher risk of having a severe case of chickenpox such as people over 12 years old, adults, people with immune deficiencies, or people on oral or inhaled steroid medication.
If you have been exposed, and think you may qualify for acyclovir, see your doctor before you break out to discuss this, and to have a prescription ready to fill at the first sign of rash.
Giving the chickenpox vaccine at the time of exposure
For children and adults with no history of the illness or vaccine, giving the chickenpox vaccine within 72 hours of exposure (before you even break out with the rash) has been shown to either prevent or decrease the severity of the illness. If more than 3 days have passed since exposure, it is probably best not to get the vaccine then.
CHICKENPOX VACCINE
Click here on chickenpox vaccine for a detailed discussion on the pros and cons of getting this vaccine.
Image from Prevention.com (there are lots of really gross chickenpox images out there! Luckily for you, I chose the cutest, least nausiating one!) As a side note, in their article “Vaccine Fears and Facts” they write:
The fallout: Life-threatening childhood diseases are making comebacks. There were 11,647 cases of whooping cough (pertussis) last year, up from 1,707 in 1980, and 13 kids died from it. When a measles outbreak swept through a Pennsylvania boarding school in 2003, a pair of twins–unvaccinated for religious reasons–required hospitalization. Seven others at the school got sick. A national resurgence of measles, which infected 55,467 people and killed 166 between 1989 and 1991, started in Houston, a city with one of the country’s lowest immunization rates.
“Without mass immunizations, children today can die of diseases that killed kids as recently as 20 years ago,” warns Ditchek. “These deaths are unnecessary.”
Additionally, the vaccine-autism controversy has proven to be much ado about nothing. In any case, the questionable ingredient, thimerosal, has been removed from most vaccines (ask your doctor about it if you are still concerned.) Do yourself, your kids, and the people around you a favor. Get immunized.




